This is a question we are frequently asked by dentists and hygienists. It is
critical to the survival of the implant that a routine maintenance regimen be adhered to.
To improve the long term success of implants, certain hygiene techniques,
instrumentation and the use of antimicrobial agents are recommended.
A study of various oral hygiene instruments found that the interdental brush, plastic
scaler and prophylactic cup all left the implant surface smooth, whereas the surface was
severely roughened by ultrasonic instrumentation and metal curettes. Air powered
abrasives, such as a prophy-jet, have been shown not to effect the implant surface, while
effectively removing microorganisms. One must exercise caution not direct the pressured
spray directly into the gingival cuff. Keeping the implant and abutment as smooth as
possible is an important goal. A smooth surface tends to be less plaque retentive.
We recommend that minimal instrumentation be done on an implant demonstrating a healthy
gingival attachment as evidenced by a lack of erythema or bleeding upon gentle probing.
Remember, the soft tissues coronal to the implant-bone interface do not "attach"
to the abutment head. At best, an adherent, soft tissue cuff is formed. The soft tissue
adaptation or "cuff" is the only obstacle to the ingress of bacteria. [top]
It is important to remember that the patient may be hesitant to perform proper oral
hygiene procedures in the implant area and that area must be considered weaker due to the
lack of connective tissue fiber attachment. Therefore, subgingival instrumentation is
rendered judiciously. We can supply you with names of vendors who manufacture instruments
acceptable for debridement of this delicate interface.
Applications of antimicrobials result in no alteration of the implant surface. One
effective means of maintaining soft tissue health around the implant is the use of a rinse
such as a chlorhexidine(Peridex or Periogard), chlorine dioxide (OxyFresh), or a phenolic product (Listerine). At home, hygiene
may also benefit from the use of interdental brushes or uni-tufted brushes. A dentifrice
containing triclosan (Colgate-Total) is now available and would be advisable. If
retrievable, the superstructure should be removed at least every 18 to 24 months. This
will afford an improved access for debridement and accurate assessments of probing depths
and mobility. Additionally, regular radiographs are advisable to check for cratering. [top]
Treatment for Failing Implants:
Two Failing H.A. Coated Implants: 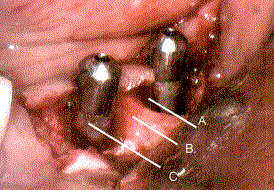
- A.--- A circumferential bony crater.
- B.--- Alveolar bone.
- C.--- HA coated implant with calculus.
Failing dental implants usually display the clinical characteristics of periodontally
diseased teeth. Progressive bone loss, pocket formation, bleeding upon probing, and
purulence are some of the findings you may notice. Successful and prompt management of the
failing implant is critical to prevent the implant loss. A failed implant is one that
displays mobility, has lost it's osseointegration and has a hopeless prognosis. Since
failed implants are functionless they should be removed so that the alveolar defect can
fill.
The subgingival microflora around a failing implant is similar to that found around
periodontally diseased teeth. Therefore, the implant surface affected by peri-implantitis
is contaminated by bacterial products , such as endotoxins, that can interfere with
biologic repair.
One must realize that a failing implant will soon become a failed implant if
intervention is not attempted. The same caution employed to minimize the roughening of the
implant and abutment is thus considered to be less important than the thorough debridement
of the effected surfaces. Calculus is often present, especially on hydroxylapatite coated
implants. It has to be removed completely. Curettes and ultrasonic instrumentation is
often employed. [top]
Chemical disinfection has been researched to remove the endotoxins. Chlorhexidine,
citric acid, hydrogen peroxide, stannous fluoride, sterile saline and tetracycline are
some of the agents which have been studied. The clinical efficacy of any of these agents
remains to be ellucidated.
Usually, these debridement procedures have to be accomplished by open flap procedures.
Adequate access is extremely important to effectively debride and detoxify the implant and
abutment. Also, this affords the opportunity to remove any inflamed granulation tissue
around the implant.
If the peri-implant supporting bone is severely cratered, bone regeneration may be
attempted if the implant has not yet lost it's integration. We advise removing the
super-structure and replacing the small healing screw. This will allow the soft tissue to
grow over the implant such that a primary closure of the soft issue flaps is easily
accomplished. Bone regenerative techniques are employed usually by placing allograft bone
into the defect and covering the implant with a resorbable guided tissue regeneration
membrane. We advise not loading the implant until the bone repair is completed. Usually
three months is required for maturation.
Finally, by definition, a failed implant is one which has lost it's integration.
Unfortunately, at this point, removal is the only solution. If in the future, the patient
is interested attempting another implant, bone regenerative methods may be employed at the
time of removal and may provide an adequate placement site after an adequate healing
period has passed. [top]